Many neurological disorders like Parkinson’s, chronic depression and other psychiatric conditions could be managed at home, thanks to a collaborative project involving researchers at the University of Queensland (UQ).
Queensland Brain Institute (QBI) Professor Peter Silburn AM said his team, together with Neurosciences Queensland and Abbott Neuromodulation have developed a remote care platform which allows patients to access treatment from anywhere in the world.
“By creating the world’s first integrated and completely wireless remote care platform, we have removed the need for patients to see their doctor in person to have their device adjusted,” Professor Silburn said.
Platform to lead to better treatment plan
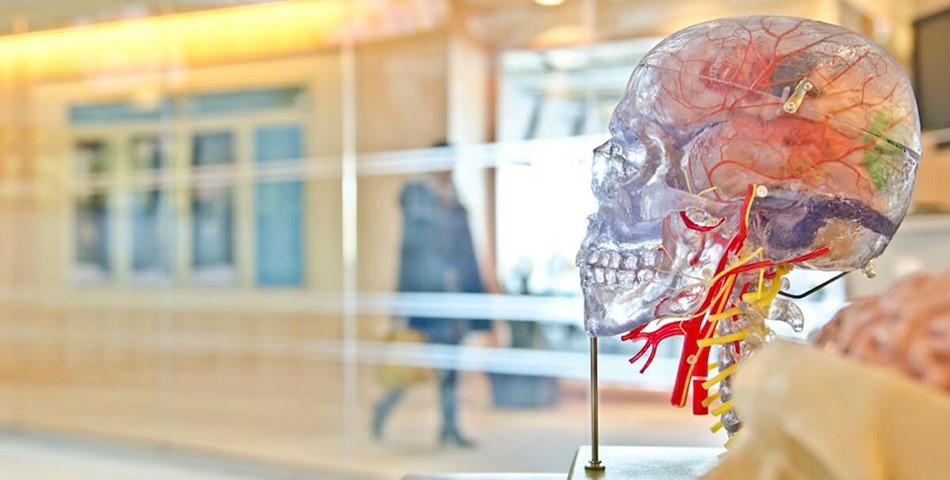
Electrodes are surgically inserted into the brain and electrical stimulation is delivered by a pacemaker which alters brain function – providing therapeutic relief and improving quality of life.
This digital platform allows clinicians to monitor patients remotely, as well as adjust the device to treat and alleviate symptoms in real time.
“We have shown that it is possible to minimise disruption to patients’ and carers’ lifestyles by increasing accessibility to the service, saving time and money,” Professor Silburn said.
“There are no cures for many of these conditions which often require life-long treatment and care, so for those people the device would be a game-changer.”
He said the system also fostered increasingly personalised treatment and data-driven clinical decisions, which could improve patient care.
“During the study, we established the platform safety, security, usability and effectiveness and optimised its features using patient feedback in a biodesign process,” Professor Silburn said.
“In the initial weeks of a limited market release, we conducted 858 remote care sessions and maintained a robust and high success rate.”
Future to bring advances in neuromodulation
While the team started working on this digital health solution before COVID-19, the pandemic elevated the need for remote care platforms, particularly for older people and those living in remote areas with increased travel difficulties.
“Through the pandemic patients have become more familiar with telemedicine and far more willing to adapt to platforms that connect them remotely to their healthcare teams,” Professor Silburn said.
The researchers are confident the technology could be adapted for many other conditions in the future.
“As we discover more about the biomarkers in brain-related disorders, we will refine neuromodulation systems to improve treatment for neuropsychiatric disorders like depression, obsessive-compulsive disorder, anorexia and Tourette’s syndrome, to name a just a few,” Professor Silburn said.
The digital health platform for remote neuromodulation systems has regulatory approval and launched in Australia in October 2021.
It has also been adopted in the United States by the Food and Drug Administration Service and the European CE-Mark.
Professor Silburn and QBI Director Professor Pankaj Sah and Associate Professor Terry Coyne will present at a series of information sessions for patients and carers living with Parkinson’s Disease, Dystonia, Essential Tremor and Tourette’s Syndrome in regional Queensland in the coming months.
The telemedicine market was valued at approximately just over US$104 billion in 2021, and it is projected to grow to roughly US$272 billion in 2027, recording a CAGR of 20.5% over the forecast period 2022-2027.
Telehealth has emerged as an essential component of healthcare as a result of the COVID-19 pandemic. Research from 2020 found that during the SARS-CoV-2 pandemic, physical distancing was put in place to minimise the spread of the coronavirus disease. This resulted in the adoption of telemedicine for most outpatient oncology appointments.
While telemedicine services were integrated into most healthcare systems even before the onset of the pandemic, services began to be extensively used only during the COVID-19 crisis. This is attributed mostly to a lack of in-person visits and limitations and restrictions on travel, which encouraged clinicians to adapt telemedicine-based consultations even more during the pandemic. Thus, the COVID-19 pandemic is expected to have a significant positive impact on the growth of the telemedicine market across the globe.
Abstract
Electroceutical therapies using electronic devices for stimulating and recording activity in the nervous system are under development or in use for a large variety of diseases affecting the nervous system or other organs. This chapter focuses on the electroceutical strategies applied to acquired injuries of the nervous system. Electrical stimulation therapies have been proposed for promoting neural repair and regeneration after injury, and for modulating neural plasticity mechanisms that may assist to recover lost functions. Acute electrical stimulation of injured peripheral nerves has been shown to accelerate axonal regeneration and enhance functional connections, as well as to modulate dysfunctions in spinal cord excitability. Bioelectronic devices that provide electrical stimulation to either promote regeneration of the injured spinal tracts or to activate preserved spinal circuits below the injury, have opened new paradigms for spinal cord injury therapy. Electrostimulation has also been used to restore the excitatory-inhibitory balance of the brain and to reorganize neural circuits in the treatment of neurological disorders. Noninvasive cortical stimulation has been included in rehabilitation programs, complementing physical therapy, with substantial improvement in cortical plasticity and functional recover